What is Infertility?
Infertility is defined by the failure to achieve a clinical pregnancy in 1 year of regular unprotected sexual intercourse.
Therefore, recently the word 'Subfertility' is used instead of infertility.
When is the right time to have examination?
If the both partners are healthy and young, under the age of 30, it is recommended to wait for one more year.
If they have not sufficient sexual intercourses, they may need to wait for two years.
However, women over the age of 35 have been trying to conceive for 6 months without success, a visit to an infertility center could be helpful. It is recommended the male partner takes a semen quality test as well.
What are the causes of infertility?
Infertility can be caused if there any interruptions and structural abnormalities on any stages of pregnancy, production of reproductive cells for either or both male and female (sperm and egg), fertilization of sperm and egg, development of fertilized egg and importing into the uterus of fertilized egg.
Causes in Females 1.Fallopian tubal factors 2.Ovulatory factors 3.Peritoneal factors 4.Anatomical factors 5.Congenital factors 6.Immunologic factors | Causes in Males 1.Spermatogenetic problems 2.Deferent duct problems 3.Pathological disorders 4.Congenital disorders 5.Functional disorders |
When is the right time to have examination?
Tests on Females
 | Basic examination |
 | Hormone Examination |
 | Hysterosalpingogram : HSG |
 | Ovulation Test |
 | Postcoital Test (PCT) |
 | Progesterone Test & Endometrial Biopsy |
 | Diagnostic Laparoscopy |
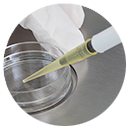 | Diagnostic Hysteroscopy |
 | Anti-Mullerian Hormone (AMH) |
Tests on Males
 | Basic examination |
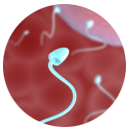 | Examination of Semen |
Information of Treatment
We provide useful and helpful information of fertility treatment
We offer to patients a wide range of safe fertility treatment options including Intrauterine Insemination,
In-vitro Fertilization and Intra-cytoplasmic Sperm Injection.
Intrauterine Insemination
Intrauterine Insemination, also known as artificial insemination, is a fertility procedure in which sperm is injected directly in woman's vagina, cervical canal, Fallopian tubes or uterus. It is the most common fertility procedure.
In-Vitro Fertilization
In-Vitro Fertilization and Embryo Transfer were firstly introduced for the female patients who became infertile because of physical cause such as Fallopian tube disorder and their objects are recently expanded to the infertility by unknown cause, immunologic factor, endometriosis, cervical factor, ovarian dysfunction and the male infertility.
In-Vitro Fertilization is a process of recruiting multiple eggs matured by controlled ovarian from the woman's ovaries and combining with sperm outside of the body, in-vitro. The cultured fertilized eggs are then transferred to the woman's uterus using long thin catheter.
Intro-cytoplasmic Sperm Injection
Intro-cytoplasmic Sperm Injection is a fertilization procedure in which a single sperm is injected directly to the cytoplasm of an egg, using the micropipette, of which internal diameter is smaller than about 5μm.
It can be used in male infertilization with oligozoospermia, asthemozoospermia, teratozoospermia and oligoasthenoteratozoospermia to overcome the unfertilization or low fertilization rate.
It can be applied to increase fertilization rate in the patients who either could not succed by IVF before or have low fertilization rate.
Assisted Hatching
Assisted Hatching is a procedure of assisted reproductive technology of making a hole in the zona pellucida of the embryo or thinning the zona pellucida.
Embryo in the blastocyst stage is needed to be hatched, the procedure of being pushed out of the zona pellucida.
However, embryos of aged patients or having abnormally thick zona pellucida have difficulties to be implant in the uterus because of poor hatching process. It is applied to overcome such problems.
Embryo Glue
When the embryo is cultured in the embryo glue, implantation promoting medium containing highly concentrated hyaluronic acid for certain period of time, the implantation rate can increase by activating the signal system between the embryo and endometrium.
Cryopreservation *
Semen Cryopreservation
The male partner who is either apart from the female parnter for long period or needed radiation therapy may preserve sperm cells and use them for the in-vitro fertilization procedure after thawing.
For the patient with aspernia, semen can be obtained from the testicular tissues and used for fertilization procedure by using cryopreservation.
Also we run the semen bank, preserving donated semen for the patient with aspernia.
Embryo Cryopreservation
Because multiple eggs are recruited from ovarian hyperstimulation, necessity of cryopreservation of leftover embryos after a cycle of intrauterine insemination is increasing.
Embryos will be frozen by vitrification method and preserved in liquid nitrogen with temperatute of -196ºC.
Normally developed healthy embryos can be transferred directly to recepients after thawing.
*By cryopreservaion
1. Rate of plural pregnancy can decrease
2. Patients can have economical advantage by having chance to transfer embryos for multiple times with one controlled ovarian and cumulative pregnancy rate can increase
3. Embryo transfer can be postponed for the patients with ovarian hyperstimulation syndrome (OHSS) to prevent severe and critical side effects and to expect safe pregnancy later